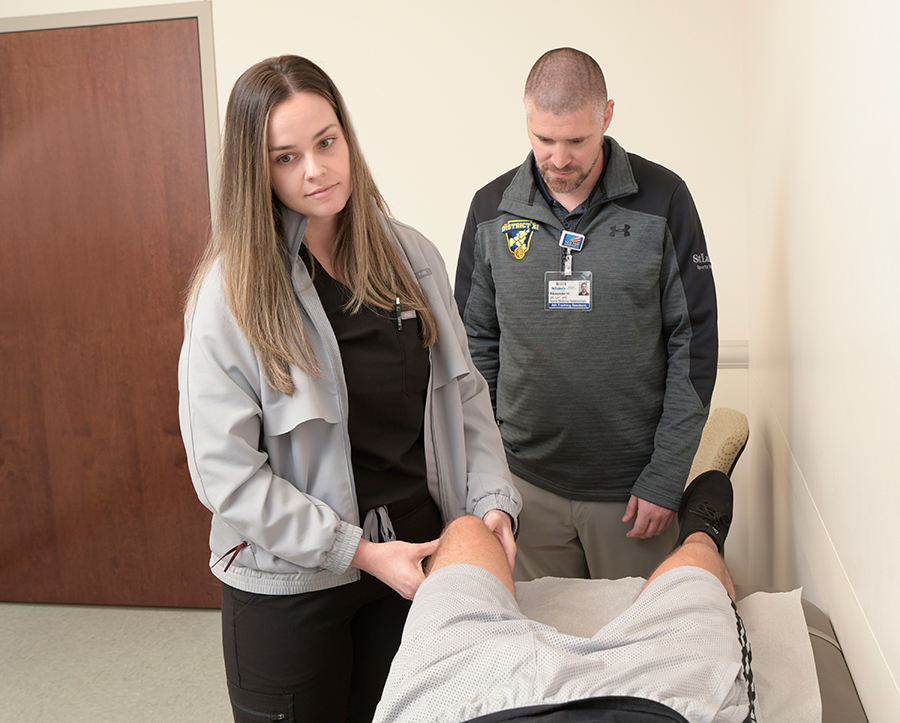
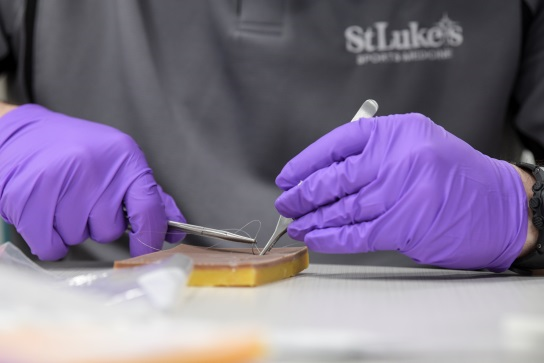
- Develop practitioners with advanced clinical skills to optimize patient outcomes within orthopedic practice.
- Develop leaders who advocate for quality and equitable patient care within inter-professional healthcare teams, analyze the efficacy of medical intervention, and enhance safety by identifying errors and implementing potential system solutions.
- Develop thinkers, who systematically analyze self-practice by identifying strengths and limitations, who set learning and improvement goals by incorporating formative evaluation feedback to guide personal and professional development
Curriculum
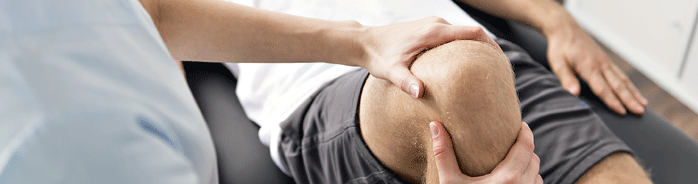
-
-
Upon completion of this residency, the athletic trainer will:
- Demonstrate cultural and social competence by recognizing that diverse perspectives and backgrounds strengthen approaches to solving social problems and contribute to improved communication, advocacy, and outcomes for our patients.
- Develop, guide, and evaluate professional and community health education initiatives that disseminates new knowledge and/or policy which will directly affect the population served.
- Devise and continually modify individualized developmental plans (IDP) that will allow for systematic self-analysis to foster self-directed, self-monitored, and self-corrective learning and thinking.
- Demonstrate professional leadership in promoting the appropriate utilization and completion of health records while capturing patient reported outcomes.
- Construct clinically relevant questions, gather and critically appraise evidence to develop solutions that incorporate principles of evidence-based care and information mastery into clinical practice.
- Perform multi-cycle quality improvement initiatives to address identified weaknesses of the system and suggest solutions to improve health care quality and optimal patient care systems.
- Perform comprehensive patient assessments targeting chief complaints, while accounting for unique circumstances, comorbidities, and historical subtleties, to formulate a list of differential diagnoses guiding diagnostic testing for simple and complex conditions across a spectrum of ages and impairments.
- Interpret diagnostic testing (e.g. plain radiographs, MRI, MR Arthrograms, NCS, EMG, CMP, and CBC) and physical examination findings to develop unique care plans which prioritize the patient’s interests and are prudent to the risks and benefits associated with common and complex procedures and tests performed.
- Collaborate with the attending physician to manage simple and complex orthopedic patients and when needed modify care plans, to maximize long-term health-related quality of life measures.
Residents will progress through didactic and immersive experiences in the following modules:
Core Didactic Modules
Core Didactic and Clinical experiences will occur within the structure of five modules. These modules include:
- Core Competencies
- Evidence-Based Practice and Quality Improvement
- Musculoskeletal Evaluation, Diagnosis and Management
- Musculoskeletal Diagnostic Imaging
- Primary Care Considerations for Musculoskeletal Management
Additional Didactic Education
Formalized structured experiences focused on specific specialty skill and knowledge development within St. Luke’s University Health Network.
- Surgical Curriculum
- Leadership Curriculum