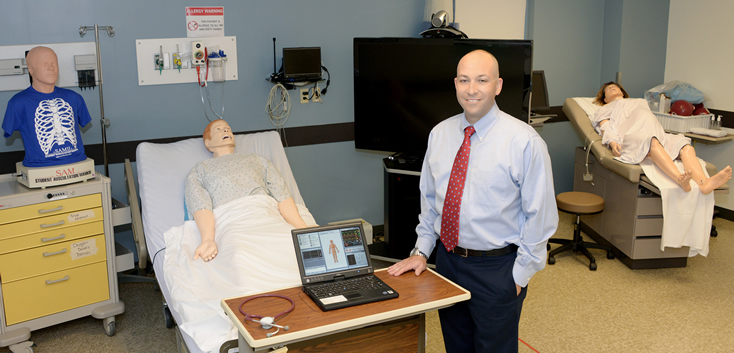
St. Luke’s Network Simulation Center
Located at St. Luke’s University Hospital – Bethlehem, the Network Simulation Center is utilized by all levels of St. Luke’s University Health Network providers for “High-Risk, Low-Volume” situations, inter-professional and competency training. Medical and nursing students from Temple/St. Luke’s School of Medicine, St. Luke’s School of Nursing, Moravian College School of Nursing and Penn State (LPN students) are provided with unique learning opportunities to develop their clinical, procedural, and professional skills.
Comprised of three state-of-the-art simulation rooms, six standardized patient exam rooms, and a clinical skills lab, simulation experiences include:
- Human Patient Simulators
- Life-Like Task Trainers
- Standardized Patients
- Objective Feedback Simulators
Safety First
The primary goal of the Simulation Center is to enhance safety within the realm of patient care. Simulation-based education provides a controlled environment that imitates a real-life patient care setting. Through simulation, learners can practice and master their skills without the risk of harm to real patients.
High fidelity, human patient simulators imitate physiologic and clinical symptoms that clinicians may encounter. Small groups of learners work together to assess the “patient’s” problem and to develop and implement a management plan or provide intervention. A faculty member observes the group, then debriefs the students about the encounter to develop their skills for future encounters with patients.
“At the only regional medical school, our simulation center is the place to make the mistakes our students will learn to not repeat in real life situations,” says Joshua Onia, M.S., CHSOS, Director, Network Simulation Center, “and it’s in the debriefing sessions afterwards — often twice the time length of the simulated event — where the deepest learning actually takes place.”
Students also develop their history-taking and physical examination skills and professional behaviors through sessions with standardized patients (actors). The opportunity to work first with standardized patients (who portray a specific patient) helps to build a student’s confidence in advance of encountering actual patients.
Life-Like/Hands-On
Human Patient Simulators (HPS) can breathe, sweat, tear, demonstrate pulses, show pulipary response, and demonstrate a variety of clinical symptoms. Patient monitors can be configured based on the level of learner to show EKG, pulse oximitry, blood pressure, arterial waveforms, labs results, and radiology reports.
Procedures including bag-mask ventilation, intubation, defibrillation, chest tube placement, and cricothyrotomy can be performed on the manikin. By practicing clinical moves in a safe and regulated environment, future physicians and nurses learn acquire key competencies, including communication, teamwork, and leadership, in addition to mastering tasks that require well-practiced manual skills such as diagnostics and surgical procedures.
Communicating
How a medical professional conducts an exam is vital, both from a clinical and communication perspective. Simulating common doctor/patient interactions that take place every day develops better communication skills.
Standardized Patient encounters involve the use of individuals trained to portray the role of a patient, family member, and others, enabling medical and nursing students to practice physical exam skills, history taking skills, diagnostic skills, and communication skills. A Standardized Patient is a person carefully recruited and trained to portray a real patient, affording the student an opportunity to learn and to be evaluated in a simulated clinical environment. Many scenarios include simulated physical symptoms, such as abdominal pain, back pain, fatigue, stroke, or a heart attack. Standardized Patients also portray patients who may have underlying findings, such as being a victim of domestic violence, suffering from substance abuse, or be going through sexual transition. The simulations give students the opportunity to practice delivering serious and possibly difficult-to-accept information, including the death of a loved one, the unlikelihood of recovery, or the discovery of an abnormal genetic or metabolic problem — before having to deliver actual bad news to real patients, and with all cases originating from real patient experiences.
Contact
To learn more about Network Simulation Center, contact:
Joshua Onia, M.S., CHSOS
Director, Network Simulation Center
Phone: 484-526-8870
Email: Joshua.Onia@sluhn.org